Clear and Breezy, 59° F
I personally and professionally have struggled with how to think about the novel 2019 coronavirus disease (COVID-19).
Let me share with you where I am with COVID-19: It is a real pandemic; our …
This item is available in full to subscribers.
The Powell Tribune has expanded its online content. To continue reading, you will need to either log in to your subscriber account, or purchase a subscription.
If you are a current print subscriber, you can set up a free web account by clicking here.
If you already have a web account, but need to reset it, you can do so by clicking here.
If you would like to purchase a subscription click here.
Please log in to continue |
|
I personally and professionally have struggled with how to think about the novel 2019 coronavirus disease (COVID-19).
Let me share with you where I am with COVID-19: It is a real pandemic; our government’s drastic efforts at containment measures are necessary; the containment measures are sincere efforts to help the American people. Why do I say this? Settle in, because we are going to have to put on our thinking caps.
First, we need to talk statistics. I have seen multiple people post influenza statistics, which are fairly shocking when we are talking about 35.5 million illnesses and 34,200 deaths in the 2018-2019 influenza season in the United States. That total number is substantial, and we admittedly should work harder to decrease that number. However, are we comparing apples to apples when we talk about influenza and COVID-19? The initial statistics would say no.
There are two main characteristics of a virus/disease we need to look at: 1) the attack rate and 2) the fatality rate. The following data and thoughts come from “2019-nCov Epidemiology: What Do These Numbers Really Mean?” by Dr. F. Perry Wilson, published by MedScape on Feb. 11.
Attack rate: The “attack rate” is essentially the contagiousness of the virus. The visual in the article uses a single infected person in close contact with five people (each person is a representation of 20%). A rate of one means the infected person on average would pass the virus to one of the five people, which would be 20%. A 20% attack rate would keep an infection active in a community, but not necessarily growing. An attack rate of less than 1, then, would indicate an infection that slowly would peter out. A rate of greater than 1 would be an infection with potential to exponentially spread, because one person spreads to more than one of those five people represented and would be a rate greater than 20%.
In real life, influenza has an attack rate around 1.5. So one infected person can spread the disease to 30% of people in close contact. At the time of this cited article in early February, the attack rate for COVID-19 was estimated to be around 2.5 — or 50%. So, these numbers would indicate COVID-19 has the potential to spread to more people than influenza.
Fatality rate: The “fatality rate” is the percentage of INFECTED people who die from the disease. Influenza has a fatality rate of 0.1%, which means for every 1,000 people who contract influenza, one person would die. For comparison, the Spanish Flu had a fatality rate of 10%, so one person out of each 10 infected people would die.
So where does COVID-19 fall on the scale? Early reports pegged the number at 2-3%, or two to three out of every 100 infected people! However, this number is evolving and apparently decreasing, while scientists estimate the rate will finalize between 0.5 to 2%.
Factors that I think will move the needle up or down:
• Testing: The number of cases in the population, especially the US, are drastically higher than test-confirmed cases due to the delayed rollout of testing kits — so the fatality rate should drive significantly lower for this reason.
• Mitigation methods: Initial estimates for the attack rate and fatality rate, of course, came out of China. Can we trust their numbers? Could their reported fatality rate of 3% be the best case scenario?
The one factor I have not heard anyone talk about when comparing China to the U.S. is how China stopped the initial exponential spread of the disease. They used military policing action to lock down Wuhan — a city of 11 million people — to slow the initial spread. Four months into this pandemic and reportedly China has a significantly decreased rate of spread.
In comparison, the U.S. is canceling sporting events and large groupings of people; travel is largely unrestricted. I have a suspicion that our attack rate with the solution of “social distancing” is going to be significantly different when compared to a military lockdown.
So, let’s go back to the comments I am hearing about more people dying from influenza than COVID-19. Technically, as of this writing, more people have died this winter from influenza than COVID-19. However, let’s say we had just the same amount of COVID-19 cases as influenza cases, with a fatality rate that is five to 20 times greater (0.1% compared to 0.5-2%). That would take that death toll of 35,000 from influenza up to 175,000 on the low side to 700,000 on the high side from COVID-19.
However, that is using the same amount of total illness cases of 35.5 million. Will we have that many cases of COVID-19 infection? Will we have even more cases if we factor in an attack rate of 2.5 instead of 1.5? We just don’t know.
Now, we do need to factor in that COVID-19 disease severity and mortality is drastically higher in the elderly while much more mild in kids. That’s great news for all of you young families and kids. This is not good news for our elderly population.
If we think back to the previous paragraph, instead of an infection rate spread across an entire population, consider what might be the fatality rate from just the elderly population? The mortality rate cannot remain at 0.5-2% for the elderly. In China, this rate was calculated to be 14.8% for those 80 years old and older.
So, let’s give those statistics a face and a place: the Kirkland Life Care Center nursing home outside of Seattle. We have all heard about it, but have we really heard about it?
Here is the story by the numbers:
These numbers calculate out to be an attack rate around 50% and a fatality rate ranging from a low of 25% up to a high of nearly 50%, depending on how you count the non-tested patients.
Let’s finally pull this all together and discuss how COVID-19 could overwhelm Wyoming’s healthcare system. Just think, every small town in Wyoming that has a small hospital has a small ICU with two, three, maybe five ventilators throughout the whole facility. Now, take just the elderly in that town’s small nursing home and give them a sprinkling of COVID-19. Those five ventilators will now be in use.
What happens with the rest of the elderly living in the community? What happens to the high school student injured in a car accident who is intubated and needs to be placed on a ventilator? What happens to a child who has a bad asthma attack and needs CPAP or intubation in order to breathe? One country is now having to answer these questions every day: Medical professionals in Italy are having to decide who is worthy of the ventilator and who is not. In the article, “The Extraordinary Decisions Facing Italian Doctors,” published on March 11 in The Atlantic magazine, author Yascha Mounk delves into this untenable but inescapable scenario.
Right now, you may be saying, “C’mon doc, you are just trying to scare me. Surely we have plenty of ICU rooms and ventilators … we live in America!” But do we? In her March 4 article published by MedScape, “Flood Of COVID-19 Patients Could Swamp Hospitals,” Brenda Goodman analyzes the numbers and sounds the alarm bells for those who will listen.
Here in Powell, we have three residential living communities for our elderly relatives. In our hospital, we have two ICU beds. No matter how you run the numbers, this is emotionally and ethically tough math.
I know we are all frustrated with canceled sporting events, concerts, schools, gatherings, and vacations. We are frustrated with our retirement accounts. We are frustrated there isn’t toilet paper on the shelves.
If this virus is going to spread, many ask, why fight against it since it will be mild for so many of us? Some might even say, “Let’s just get it over with — like a chickenpox party.”
But fight it we must — if we love our grandparents, our parents, uncles and aunts, our mentors and co-workers; if we don’t want to experience a death rate of 2.5% or higher; if we don’t want our doctors and nurses to have to ration life-saving medical care. That said, we can not necessarily stop the spread of COVID-19, but we can try to slow the spread.
We can try to keep it from hitting all of our elderly folks at once. We can try to spread the demand on the healthcare system over a period of time instead of one big rush on resources. This “try” has come to be known as “flattening the curve” and is described in the article, “Flattening The Coronavirus Curve” by Siobhan Roberts in the New York Times on March 11.
I hope this helps. Let’s think big picture. Let’s not be afraid — but let’s be prudent.
Godspeed.
(Dr. Dean Bartholomew is a physician with 307Health — a direct primary care medical practice in Powell — and a former president of the Wyoming Medical Society and Wyoming Academy of Family Physicians. Karrie Tracy, 307Health’s business manager, helped compose this piece.)
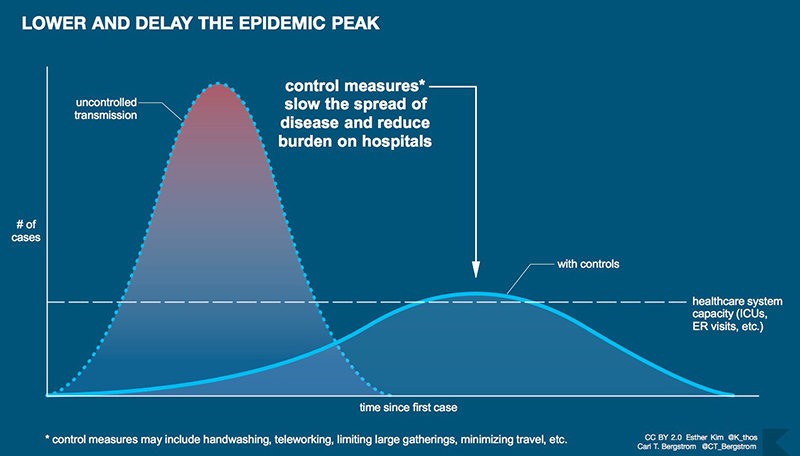
This graphic shows how taking precautionary measures can theoretically slow the spread of COVID-19 and avoid swamping the health care system.
Image courtesy Esther Kim and Carl T. Bergstrom